Professional vs Institutional Claims in Medical Billing: Key Differences Explained
Introduction
In medical billing, submitting accurate claims is essential for timely reimbursement and maintaining a healthy revenue cycle. One of the most important concepts billing professionals must understand is the difference between professional vs institutional claims in medical billing.
At RevenueCtrl LLC, we help healthcare providers simplify complex billing processes and ensure maximum reimbursement with minimal errors.
What Are Professional Claims?
Professional claims are used for services provided by individual healthcare professionals such as physicians, therapists, and specialists. These services are usually performed in outpatient settings like clinics, offices, or even patient homes.
Examples of Professional Services:
- Office visits
- Consultations
- Diagnostic tests
- Minor procedures
Key Features of Professional Claims:
- Linked to individual providers
- Mostly outpatient services
- Submitted using the CMS-1500 form
- Include CPT and ICD-10 codes
What Are Institutional Claims?
Institutional claims are submitted by healthcare facilities such as hospitals, nursing homes, and rehabilitation centers. These claims cover a wide range of services, including both inpatient and outpatient care.
Examples of Institutional Services:
- Hospital stays (inpatient care)
- Emergency room visits
- Outpatient surgeries
- Diagnostic imaging
Key Features of Institutional Claims:
- Associated with healthcare facilities
- Covers inpatient and outpatient services
- Submitted using the UB-04 form
- Includes detailed facility and service data
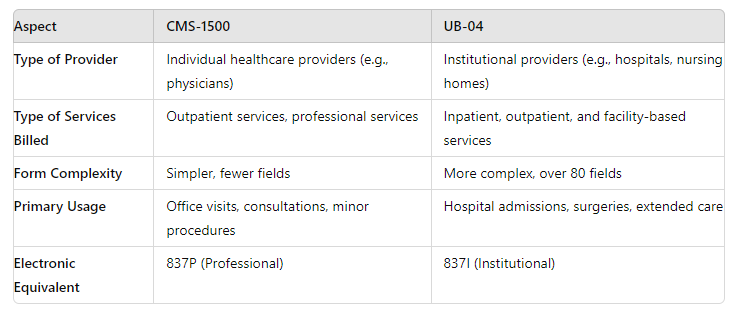
Key Differences Between Professional and Institutional Claims
| Feature | Professional Claims | Institutional Claims |
|---|---|---|
| Provider Type | Individual providers | Healthcare facilities |
| Service Location | Clinics, offices | Hospitals, centers |
| Type of Care | Outpatient only | Inpatient & outpatient |
| Billing Form | CMS-1500 | UB-04 |
| Complexity | Moderate | High |
Why Understanding This Difference Matters
Understanding the distinction between these two claim types is crucial for:
Accurate Billing
Submitting the correct claim type ensures proper reimbursement.
Reduced Claim Denials
Using the wrong form or data can lead to rejections.
Faster Payments
Correct claims processing leads to quicker reimbursements.
Compliance with Regulations
Helps avoid compliance issues with insurance providers.
Common Mistakes to Avoid
- Using the wrong billing form
- Misclassifying services
- Incorrect coding
- Missing facility or provider details
- Incomplete documentation
Avoiding these mistakes can significantly improve your billing success rate.
How RevenueCtrl LLC Helps
At RevenueCtrl LLC, we specialize in handling both professional and institutional claims with precision.
Our Services Include:
- Accurate claim submission (CMS-1500 & UB-04)
- Coding and compliance checks
- Denial management and resubmission
- Revenue cycle optimization
- End-to-end billing support
We ensure your claims are processed correctly the first time, reducing delays and maximizing revenue.
Conclusion
Understanding professional vs institutional claims in medical billing is essential for efficient billing and revenue optimization. Each claim type has its own structure, requirements, and submission process.
By implementing best practices and working with experts like RevenueCtrl LLC, healthcare providers can streamline their billing operations and achieve faster reimbursements.